
Phototherapy for Psoriasis: Can It Help?
Psoriasis is a chronic skin condition that affects millions of people worldwide, causing red, scaly patches that can be uncomfortable and sometimes painful. While there are many approaches to managing psoriasis, it’s important to understand that no single solution works for everyone—and there is currently no cure. Phototherapy, a treatment that uses specific wavelengths of light, is sometimes recommended to help manage symptoms. However, phototherapy is not a cure or a guaranteed solution for psoriasis.
What Is Psoriasis?
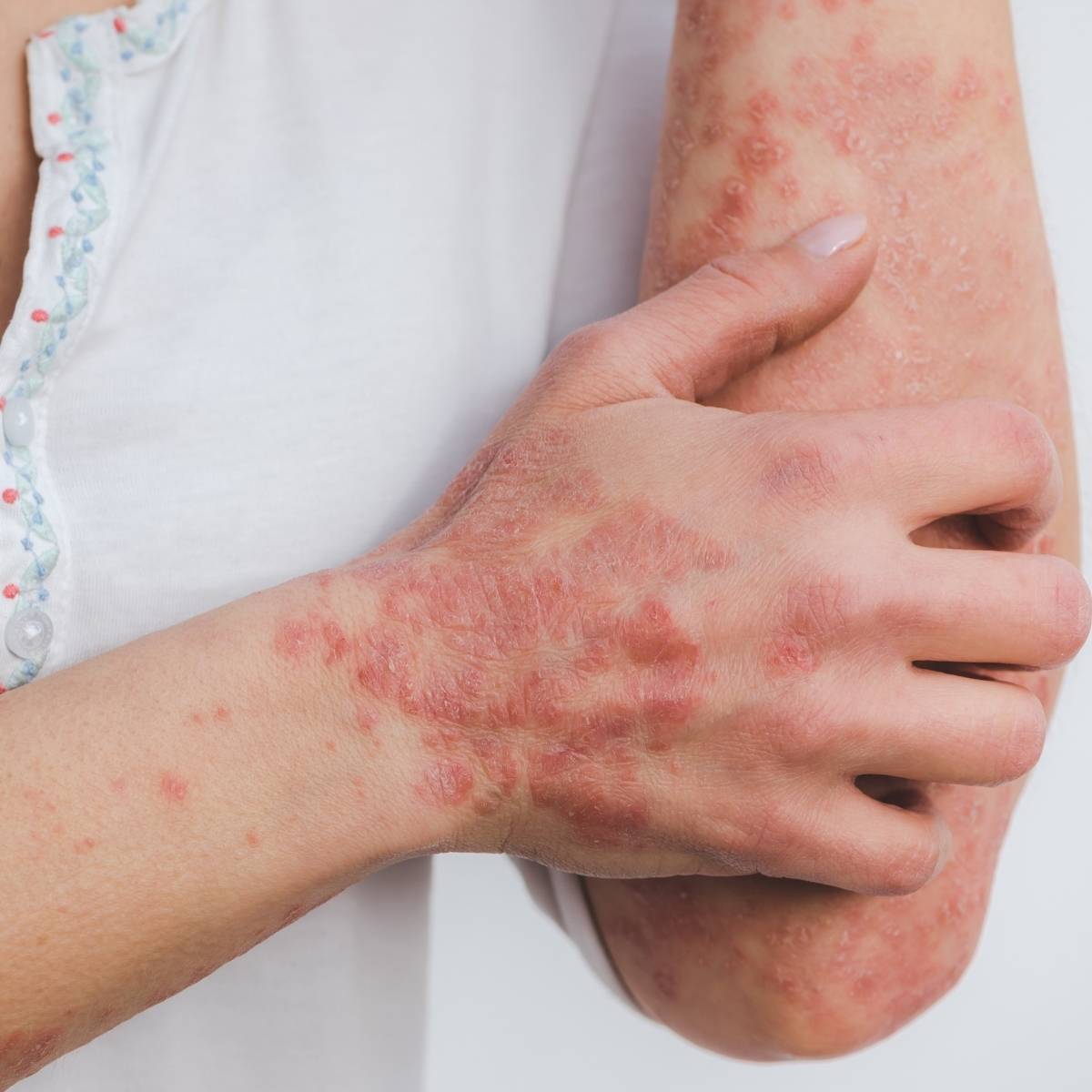
Psoriasis is a long-lasting, non-contagious skin condition that causes your immune system to become overactive, leading to the rapid growth of skin cells. Instead of shedding naturally, these extra skin cells build up on the surface, forming thick, red patches covered with silvery-white scales. These patches, known as plaques, can appear anywhere on your body but are most commonly found on the elbows, knees, scalp, and lower back. Psoriasis can range from mild, with just a few small patches, to severe, covering large areas of your skin.
The symptoms of psoriasis go beyond just the visible plaques. You might experience itching, burning, or soreness in affected areas. In some cases, the skin can crack and bleed, making daily activities uncomfortable. Some people with psoriasis also develop psoriatic arthritis, which causes joint pain and swelling.
While the exact cause of psoriasis isn’t fully understood, it’s believed to be related to a combination of genetic and environmental factors. If you have a family history of psoriasis, your risk is higher. However, not everyone with a genetic predisposition will develop the condition.
Certain triggers can set off or worsen psoriasis symptoms, including:
-
Stress: Emotional or physical stress can cause flare-ups.
-
Skin injuries: Cuts, scrapes, sunburns, or even vaccinations can trigger new patches.
-
Infections: Throat infections, especially strep throat, are known to trigger psoriasis in some people.
-
Medications: Certain drugs, such as lithium, beta-blockers, and antimalarials, can worsen symptoms.
-
Weather: Cold, dry weather can make symptoms more severe, while sunlight may help some people.
-
Lifestyle factors: Smoking and heavy alcohol use are linked to more severe psoriasis.
Living with psoriasis can have a significant impact on your daily life and emotional well-being. The visible nature of the condition may affect your self-confidence and lead to feelings of embarrassment or frustration. You might find yourself avoiding social situations or certain activities, especially if your symptoms are difficult to manage. The discomfort and pain from plaques can also interfere with sleep, work, and physical activity. Over time, the ongoing nature of psoriasis and its unpredictability can contribute to anxiety, depression, or feelings of isolation.
The most common evidence-based treatments for psoriasis include topical medications, systemic therapies, and biologic drugs. Topical treatments, such as corticosteroids, vitamin D analogues, and coal tar, are often the first line of defense for mild to moderate cases and work by reducing inflammation and slowing skin cell growth. For more severe or widespread psoriasis, systemic medications—taken orally or by injection—may be prescribed. These include methotrexate, cyclosporine, and acitretin, which help control the immune system’s overactivity. Biologic drugs, a newer class of treatments, target specific parts of the immune system involved in psoriasis and are typically reserved for moderate to severe cases that haven’t responded to other therapies. In addition to these medical options, lifestyle changes like managing stress, maintaining a healthy weight, and avoiding known triggers can also play a significant role in controlling symptoms. Each treatment plan should be tailored to your individual needs and discussed with your healthcare provider.
It’s important to remember that you’re not alone—psoriasis is a common condition, and support is available.
What Is Phototherapy?
Phototherapy is a medical treatment that uses specific wavelengths of ultraviolet (UV) light to help manage certain skin conditions, including psoriasis. Unlike cosmetic light therapies such as red light therapy or blue light therapy—which are often marketed for visible wrinkle reduction or acne treatment—phototherapy for psoriasis relies on controlled exposure to UV light, which has a different mechanism and purpose.
In phototherapy, the most commonly used types of light are ultraviolet B (UVB) and ultraviolet A (UVA). These forms of light penetrate the skin at different depths and have unique effects on skin cells:
-
UVB Phototherapy: This is the most widely used form of phototherapy for psoriasis. UVB light, particularly in the narrowband range (311–313 nm), slows down the rapid growth of skin cells that leads to psoriasis plaques. Treatments are typically administered in a medical setting, where your exposure to UVB light is carefully monitored to minimize risks.
-
PUVA Therapy: PUVA stands for Psoralen combined with UVA light. In this treatment, you take a medication called psoralen (either orally or applied to the skin), which makes your skin more sensitive to UVA light. Then, your skin is exposed to UVA rays. PUVA is generally reserved for more severe cases of psoriasis or when other treatments haven’t been effective, as it carries a higher risk of side effects.
-
Excimer Laser: This is a targeted form of UVB therapy that uses a focused beam of light to treat specific, stubborn plaques without exposing the surrounding healthy skin. The excimer laser is often used for small, localized areas of psoriasis.
The way phototherapy works is by slowing the overactive growth of skin cells and reducing inflammation. When your skin is exposed to controlled doses of UV light, it can help normalize cell turnover and decrease the scaling and thickness of plaques. However, the effects are temporary, and regular sessions are usually needed to maintain results.
Is Phototherapy Effective for Psoriasis?
Phototherapy has been studied extensively as a treatment option for psoriasis, and research shows that it can help reduce symptoms for many people. Clinical evidence suggests that both UVB and PUVA phototherapy can lead to significant improvements in plaque thickness, redness, and scaling. Many patients experience periods of clearer skin and relief from itching and discomfort after a series of treatments. However, it’s important to remember that results vary from person to person, and phototherapy is not a cure for psoriasis.
The benefits of phototherapy include its ability to target large or widespread areas of psoriasis, especially when topical treatments alone are not effective. Phototherapy can be a good option if you have moderate to severe psoriasis or if your symptoms are not well controlled with creams and ointments. It is also considered safe for long-term use when administered under medical supervision, and it does not involve systemic medications that may have more serious side effects.
Despite its benefits, phototherapy does have limitations. The treatment requires a significant time commitment, as you may need to visit a clinic two to three times per week for several weeks or months. Some people experience side effects such as redness, itching, or a sunburn-like reaction. Long-term use of phototherapy, especially PUVA, may increase your risk of skin aging and certain types of skin cancer. Not everyone responds to phototherapy, and some individuals may find their symptoms return quickly after stopping treatment.
It’s important to note that phototherapy for psoriasis is a medical procedure and should always be supervised by a healthcare professional. The UV light used in phototherapy is much stronger and more targeted than the light used in cosmetic devices for wrinkle reduction or acne. While red light therapy and blue light therapy are popular for their cosmetic benefits, they have not been proven effective for managing psoriasis and should not be confused with medical phototherapy.
If you’re considering phototherapy, your healthcare provider will assess your skin type, the severity of your psoriasis, and any other health factors to determine if this treatment is appropriate for you. Phototherapy is not a cure for psoriasis, but it can be a valuable part of a comprehensive management plan for some individuals. Your provider will help you weigh the potential benefits and risks, and together you can decide if phototherapy fits your needs and lifestyle.
Conclusion
Phototherapy is not a cure for psoriasis, but it can be a helpful tool for managing symptoms in some individuals. By using controlled doses of ultraviolet light under medical supervision, phototherapy may reduce the severity of plaques and provide relief from discomfort. However, it’s important to remember that results vary, and this approach is not suitable for everyone. There are many proven ways to address psoriasis, including topical treatments, systemic medications, and lifestyle changes. Working closely with your healthcare provider is essential to find the best combination of strategies for your unique needs. Always discuss your options and any concerns with a medical professional before starting new treatments. This article is intended for informational purposes only and should not be considered medical advice. Your healthcare provider is your best resource for guidance on managing psoriasis and improving your quality of life.
Disclaimer: This article is intended for informational purposes only and should not be interpreted as medical advice or guidance. Always seek medical advice and care from a trusted healthcare professional.
Sources:






















